USA Guide to Billing for Mental Health Services: How Providers Can Improve Revenue and Reduce Claim Denials
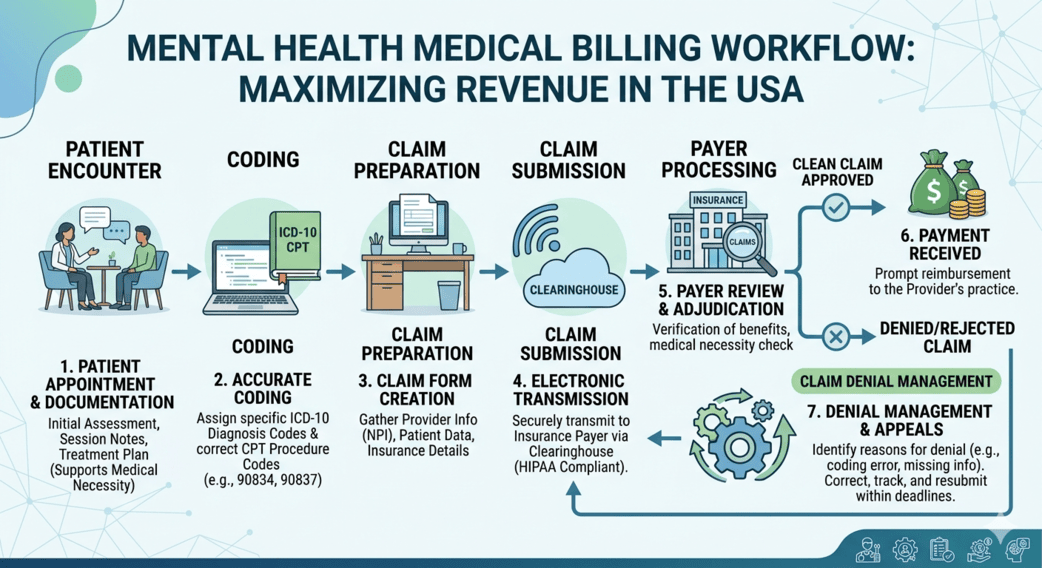
Mental health practices across the USA are facing growing pressure to balance patient care with increasingly complex administrative responsibilities. From changing payer regulations to evolving telehealth policies, billing for mental health services has become more challenging than ever. Even experienced therapists, psychiatrists, psychologists, and counseling centers often struggle with delayed reimbursements, coding errors, and insurance denials.
Accurate billing is no longer just an administrative task—it directly impacts practice sustainability, patient access, and long-term growth.
Whether you operate a solo therapy practice or manage a multi-provider behavioral health organization, understanding how mental health insurance billing works can help you avoid costly mistakes while improving cash flow and operational efficiency.
Why Mental Health Billing Is Different From Other Specialties
Behavioral health billing involves unique coding structures, authorization requirements, and payer-specific documentation standards. Unlike many traditional specialties, mental health providers often deal with:
- Time-based CPT coding
- Frequent prior authorization requests
- Teletherapy compliance requirements
- Session limit restrictions
- Complex documentation audits
- Coordination between therapists and psychiatrists
Because of these challenges, many organizations now rely on specialized mental health insurance billing services rather than managing claims entirely in-house.
A qualified mental health billing specialist understands the nuances of behavioral health reimbursement and can significantly reduce administrative burden.
Common Challenges in Billing for Mental Health Services
Even highly skilled clinicians can encounter billing complications that negatively affect reimbursement cycles.
1. Incorrect CPT Code Selection
Mental health coding depends heavily on session duration, therapy type, and provider credentials. Using the wrong CPT code can lead to denials or underpayments.
Examples include:
- 90834 for 45-minute psychotherapy
- 90837 for 60-minute psychotherapy
- 90791 for psychiatric diagnostic evaluation
A reliable mental health billing and coding company ensures coding accuracy while staying updated on payer guidelines.
2. Insurance Eligibility Errors
One of the biggest revenue leaks occurs before treatment even begins. Many practices fail to verify:
- Active insurance coverage
- Copay requirements
- Session limitations
- Telehealth eligibility
- Deductible status
This is why billing services for mental health providers often include eligibility verification as part of their workflow.
3. Prior Authorization Delays
Certain insurance carriers require authorization for ongoing therapy sessions or psychiatric treatments. Missing these approvals can result in rejected claims and revenue loss.
Experienced mental health billing consultants monitor authorization timelines proactively to avoid interruptions in reimbursement.
4. Documentation Issues
Mental health documentation must align closely with billed services. Insufficient notes can trigger audits or payment recoupments.
A professional mental health billing company typically reviews documentation compliance to ensure providers meet payer expectations.
The Growing Demand for Mental Health Billing Services in the USA
The rise in behavioral health awareness has increased patient demand dramatically. However, higher patient volume also means more billing complexity.
Many providers now choose to outsource mental health billing services because internal teams often struggle to keep up with:
- Insurance rule changes
- Coding updates
- Claims follow-up
- Denial management
- Payment posting
- Compliance monitoring
An experienced mental health billing services agency can streamline these processes while helping practices focus more on patient care.
Benefits of Outsourced Mental Health Billing
Choosing outsourced mental health billing is becoming a strategic decision for many behavioral health organizations.
Improved Claim Accuracy
Specialized billers understand behavioral health coding guidelines and payer-specific rules. This reduces claim errors and increases first-pass acceptance rates.
Faster Reimbursements
A dedicated mental health billing provider submits clean claims quickly while following up aggressively on unpaid accounts.
Reduced Administrative Burden
Therapists and office staff can focus on scheduling, treatment, and patient communication instead of spending hours on insurance calls.
Better Financial Visibility
Many mental health billing companies provide reporting dashboards that help practices monitor:
- Collections
- Denial trends
- Accounts receivable
- Insurance aging
- Revenue performance
Scalability for Growing Practices
As behavioral health practices expand, billing complexity increases. Working with a top outsource mental health billing company allows providers to scale operations without hiring large in-house teams.
What to Look for in a Mental Health Billing Agency
Not all billing vendors understand the behavioral health landscape. When evaluating the best mental health billing agency, providers should consider several important factors.
Specialty Experience
Behavioral health billing differs significantly from other medical specialties. The company should have direct expertise in:
- Psychiatry billing
- Therapy billing
- Telepsychiatry claims
- Substance abuse billing
- Psychological testing
Certified Coding Knowledge
A strong mental health medical billing solution should include experienced coders familiar with ICD-10, CPT, and HCPCS updates.
Denial Management Processes
The best outsource mental health billing and coding company will actively monitor denied claims and resubmit corrected claims quickly.
Transparency and Reporting
Reliable billing partners provide detailed reporting so practices can track revenue performance in real time.
HIPAA Compliance
Since behavioral health data is highly sensitive, strict security protocols are essential.
How Telehealth Changed Mental Health Insurance Billing
Teletherapy transformed mental health delivery across the USA. While virtual care improved accessibility, it also introduced new billing challenges.
Providers must now manage:
- Telehealth modifiers
- POS code updates
- State-specific regulations
- Audio-only billing policies
- Cross-state licensing concerns
Mental health medical billing services outsourcing providers often stay ahead of these changes better than small internal billing teams.
For example, many insurers changed telehealth reimbursement rules multiple times over the past few years. Practices without specialized support struggled to keep up.
Real-World Example: How Billing Errors Impact Revenue
Consider a small therapy group with four clinicians seeing 25 patients weekly.
If just five claims per week are denied because of coding or authorization issues, the annual revenue loss could become substantial. Delayed reimbursements also create cash flow instability, making it harder to invest in staff, technology, or patient care improvements.
After switching to a mental health billing services agency, many practices report:
- Higher clean claim rates
- Reduced denials
- Faster insurance payments
- Improved patient billing accuracy
This operational stability allows providers to focus more on treatment outcomes rather than administrative stress.
The Role of Credentialing in Mental Health Billing
Insurance credentialing is often overlooked, but it directly affects reimbursement timelines.
Without proper payer enrollment, claims may be denied entirely.
Many behavioral health practices now combine:
- Credentialing services
- Revenue cycle management services
- Medical billing and coding services
into one integrated workflow.
This approach helps reduce delays and improves overall financial performance.
For newer practices, credentialing errors can delay revenue for months. Working with experienced billing professionals can prevent these costly setbacks.
Why Revenue Cycle Management Matters in Behavioral Health
Effective revenue cycle management services go beyond claim submission.
A strong RCM strategy includes:
- Insurance verification
- Patient eligibility checks
- Accurate coding
- Claim submission
- Payment posting
- Denial resolution
- Patient collections
- Financial reporting
Mental health providers who optimize their revenue cycle often experience stronger financial consistency and lower administrative overhead.
How Technology Is Improving Mental Health Billing
Modern billing platforms are helping behavioral health organizations automate repetitive tasks while improving accuracy.
Advanced mental health medical billing solutions may include:
- Automated claim scrubbing
- Real-time eligibility verification
- Electronic remittance posting
- AI-assisted coding support
- Patient payment portals
- Integrated EHR billing workflows
However, software alone is not enough. Human expertise remains essential, especially when dealing with denials and payer disputes.
That’s why many practices combine technology with outsourced mental health billing expertise.
Signs Your Practice May Need Billing Support
Many behavioral health providers wait too long before seeking outside help.
Here are common warning signs:
- Rising claim denials
- Delayed reimbursements
- High accounts receivable
- Frequent coding errors
- Staff burnout
- Insurance follow-up delays
- Inconsistent cash flow
If these issues sound familiar, partnering with a mental health billing agency could improve operational efficiency significantly.
Choosing Between In-House and Outsourced Billing
Both approaches have advantages, but outsourcing is becoming increasingly common in behavioral health.
In-House Billing
Pros:
- Direct oversight
- Internal communication
Cons:
- Staffing costs
- Training requirements
- Limited specialty expertise
- Higher turnover risk
Outsourced Billing
Pros:
- Access to specialists
- Lower administrative burden
- Improved scalability
- Faster claims management
Cons:
- Requires careful vendor selection
For many practices, outsourced mental health billing offers better long-term efficiency and financial performance.
The Importance of Compliance in Mental Health Medical Billing
Behavioral health practices face strict compliance expectations related to:
- HIPAA regulations
- Documentation standards
- Insurance audits
- Telehealth compliance
- Coding accuracy
Errors can lead not only to denials but also legal and financial penalties.
Experienced mental health billing specialists help practices maintain compliance while reducing audit risks.
Supporting Practice Growth Through Specialized Billing
As mental health demand continues to grow in the USA, providers need operational systems that support sustainable expansion.
Partnering with experts in medical billing services, medical coding services, and revenue cycle management services can help practices:
- Improve reimbursement rates
- Reduce claim delays
- Enhance operational efficiency
- Support long-term growth
- Maintain regulatory compliance
Many behavioral health organizations also integrate credentialing services into their administrative strategy to simplify payer enrollment and provider onboarding.
Companies like 247 Medical Billing Services support healthcare organizations by combining specialized behavioral health expertise with scalable billing infrastructure.
Conclusion
Managing billing for mental health services requires more than basic claim submission knowledge. Behavioral health billing involves complex coding, payer-specific rules, documentation standards, and evolving telehealth regulations.
Practices that invest in specialized support often see measurable improvements in reimbursement speed, denial reduction, and overall revenue performance.
Whether you work with a mental health billing consultant, a mental health billing provider, or a full-service mental health billing and coding company, the right partnership can help reduce administrative stress while allowing clinicians to focus on what matters most—patient care.
As behavioral health services continue expanding across the USA, practices that prioritize accurate billing, compliance, credentialing services, medical billing and coding services, and efficient revenue cycle management services will be better positioned for long-term success.
FAQs
What is billing for mental health services?
Billing for mental health services involves submitting insurance claims for psychotherapy, psychiatry, counseling, and behavioral health treatments using accurate CPT and ICD-10 codes.
Why do mental health claims get denied frequently?
Mental health claims are commonly denied because of coding errors, missing authorizations, documentation issues, or eligibility verification problems.
Should therapists outsource mental health billing?
Many therapists choose to outsource mental health billing services to reduce administrative workload, improve claim accuracy, and speed up reimbursements.
What does a mental health billing specialist do?
A mental health billing specialist handles coding, insurance verification, claim submission, denial management, payment posting, and reimbursement follow-up for behavioral health practices.
How do mental health billing companies improve revenue?
Mental health billing companies help improve clean claim rates, reduce denials, accelerate reimbursements, and optimize overall revenue cycle performance.
What services are included in mental health medical billing services?
Most mental health medical billing services include insurance verification, coding, claims submission, denial management, payment posting, reporting, and credentialing support.
- Art
- Causes
- Crafts
- Dance
- Drinks
- Film
- Fitness
- Food
- Jogos
- Gardening
- Health
- Início
- Literature
- Music
- Networking
- Outro
- Party
- Religion
- Shopping
- Sports
- Theater
- Wellness



